Integrated Behavioral Health
Integrated Behavioral Health
It is widely recognized that unaddressed Behavioral Health (BH) conditions increase suffering and total cost of care and that BH drives 60-80% of all visits to Primary Care (PC). Building and supporting the delivery of integrated behavioral health care at PCP sites is fundamental and necessary to improve quality of life and to decrease inefficient utilization of health care services and dollars.
The Care Transformation Collaborative of Rhode Island (CTC-RI) has designed, implemented and evaluated IBH models and provides workforce and practice development programs.
Integrated Behavioral Health Pilot Program Funders



3-year pilot program with 2 waves of practices
- IBH Cohort I - Feb 2016 –December 2017
- IBH Cohort II - November 2016-October 2018
Cohort 1 |
Associates in Primary Care* |
| East Bay Community Action Program (E. Providence & Newport) | |
| Providence Community Health Centers – Chafee | |
| Tri-County Community Action* | |
| Women’s Medicine Collaborative* | |
Cohort 2 |
Brown University – Governor Street |
| Coastal Medical – Hillside Family Medicine | |
| Providence Community Health Centers – Capitol Hill | |
| Providence Community Health Centers – Prairie Avenue | |
| Wood River Health Services |
*Participated in the Major Depressive Disorder Learning Collaborative
Key Program Components:
- Support culture change, workflows, billing
- UniverOnsite IBH Practice Facilitation: sal Screening: depression, anxiety, substance use disorder
- Embedded IBH Clinician : warm hand offs, pre-visit planning, huddles
- Three PDSA Cycles : screening, high ED, chronic conditions
- Quarterly Best Practice Sharing: data driven improvement, content experts
Practice Payment: $35,000 over 2 Years
| Infrastructure Payment | 1st payment: month 1 | 2nd payment: month 5 |
| $15,000 prorated per 5000 attributed lives | $10,000 | $5,000 |
| Incentive Payment | Year 1: month 12 | Year 2: month 24 |
| $10,000 each year for meeting screening targets | Depression: 70% Anxiety: 50% Substance Use Disorder: 50% |
Depression: 90% Anxiety: 70% Substance Use Disorder: 70% |
Lessons Learned
CTC conducted a qualitative research evaluation study which included interviews with the practice staff and key stakeholders with the following barriers and recommendations identified:
- Co-pays are a barrier to treatment particularly when patients obtain “same day” care from IBH and Medical provider and when patients have to pay a higher specialist behavioral health co-pay;
- Billing and coding for behavioral health in primary care is difficult to navigate; practices recommended proving them with 6 months “startup” time to prepare for implementation; Recommendations made to consider an alternative payment system for IBH in primary care; Recommend obtaining up-front commitment from systems of care to provide practices with infrastructure support (i.e. EHR, Billing and Coding, recruiting and credentialing behavioral health clinicians);
- There is a need to build the integrated behavioral health workforce;
- Onsite practice facilitation by IBH subject matter experts supports culture change for successful implementation;
- There is a need to address the needs of smaller practices who have patients with behavioral health needs who may not have the capacity to hire on site behavioral health clinicians.
The full qualitative report can be found here and the executive report here.
Results
Providers love it: “When I say how much I love having integrated behavioral health, it is that I can’t imagine primary care without it. It just makes so much sense to me to have those resources all in the same place because it is so important.” Provider indicated in the qualitative research study
Value of deliberate screening: “I’m surprised especially with the anxiety screener that there’s more out there than I knew about. I was talking to somebody yesterday. I know the patient pretty well, and the patients, if they had an issue, would tell me. But it comes up in a screener”. Provider indicated in the qualitative research study
Impact on ED use: “One of the things we identified through the program was somebody was going to the ER almost every other day and it was due to anxiety. So, he was giving tools to control that and it actually empowered him. He felt like he had taken control of the issue. And his ER visits dropped right off. He was being seen here (at the primary care practice) more frequently, but that’s OK. We’d rather he come here than go to the ER”. Practice Manager indicated in the qualitative research study
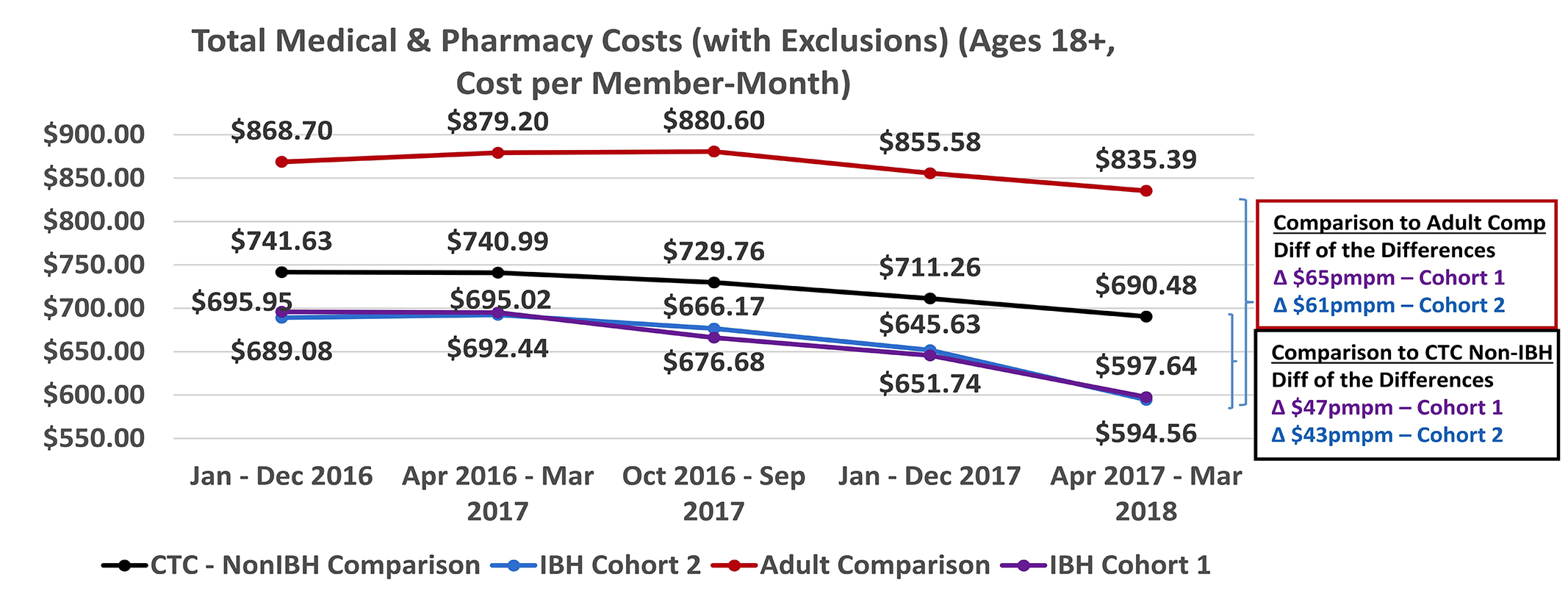
Total cost of care data from the All Payer Claims Database show significantly lower cost of care in practices that have integrated behavioral health program than the comparison groups. A more robust quantitative analysis from Brown University is due in 2020.
A presentation on the overall IBH Pilot Program can be found here (link master IBH deck).
About our support services
Having worked with over 100 pediatric, family medicine, and adult primary care practices, the Care Transformation Collaborative of Rhode Island (CTC-RI) has a proven track record for assisting primary care practices to better support the successful integration of behavioral health and primary care.
CTC-RI has received national and regional recognition and awards for our innovation and leadership. Using a personal hands-on approach, we can assist you with developing a customized action plan designed to meet your strategic objectives by offering the following integrated behavioral health services.
Care Transformation Collaborative of Rhode Island’s integrated behavioral health services include:
- Practice facilitation with seasoned content experts to integrate behavioral health care into primary care, including needs assessment, goal attainment and outcomes measurement that is evidence-based.
- Workflow and operational improvements to integrate behavioral health care into primary care needs.
- Joint staff trainings for primary care and behavioral health / substance use staff (front desk / reception, medical assistants, nursing, medical providers, behavioral health providers, and community health workers) to increase communication and care coordination for patients needing integrated behavioral health / substance use services.
- Strategies to improve referral management between Specialty Mental Health and Primary Care.
- Interactive team training on complex topics such as group visits, registry building and management, billing and coding guidance.
- Tools available - Return on Investment Financial models, Billing & Coding guidelines, scheduling templates, checklists, etc.
- Project management support for convening Learning Collaboratives with speakers and topics central to integrated behavioral health / substance use in primary car
- Implementation of SBIRT (Screening, Brief Interventions, and Referral to Treatment) in various clinical and community-based settings.
- Implementation of Community Health Teams for high-risk patients.
Practices and systems of care interested in implementing integrated behavioral health, with Dr. Nelly Burdette serving as CTC's Senior IBH leader, should contact ctcibh@ctc-ri.org.
The purpose of this training is to provide foundational knowledge and professional skills practice as preparation for individuals delivering integrated behavioral health (IBH) practice facilitation at primary care sites in Rhode Island.
Testimonial:
"The course really solidifies and celebrates the role of the practice facilitator. The resources are current and dedicated to the adult learner. You will find the experience engaging and it will expand your professional base"
Jayne Daylor RN MS.
Instructor: Nelly Burdette, Psy.D.
 Senior Integrated Behavioral Health Program Leader, Care Transformation Collaborative-Rhode Island (CTC-RI). Dr. Nelly Burdette has more than 10 years’ experience within integrated behavioral health clinical and leadership positions. She has created Integrated care programs at federally-qualified health centers, community mental health centers, and the Veteran’s Administration for pediatric, family medicine and adult populations. From positions in senior leadership to providing clinical services embedded within medical practices, she has provided integrated behavioral health training and supervision to interdisciplinary medical teams. In her current roles, Dr. Burdette is the Associate Vice President of Integrated Behavioral Health at Providence Community Health Centers, the largest federally qualified health center in Rhode Island and serves in both a leadership and clinical role. She has also been serving as a senior content expert and integrated behavioral health practice facilitator for CTC-RI for the past 4 years. Dr. Nelly Burdette received her doctorate degree in Health Psychology from Spalding University and completed her internship at Cherokee Health Systems, focusing on behavioral health services within a primary care safety net population. Her post-doctorate was completed at University of Massachusetts Medical School in Primary Care Psychology.
Senior Integrated Behavioral Health Program Leader, Care Transformation Collaborative-Rhode Island (CTC-RI). Dr. Nelly Burdette has more than 10 years’ experience within integrated behavioral health clinical and leadership positions. She has created Integrated care programs at federally-qualified health centers, community mental health centers, and the Veteran’s Administration for pediatric, family medicine and adult populations. From positions in senior leadership to providing clinical services embedded within medical practices, she has provided integrated behavioral health training and supervision to interdisciplinary medical teams. In her current roles, Dr. Burdette is the Associate Vice President of Integrated Behavioral Health at Providence Community Health Centers, the largest federally qualified health center in Rhode Island and serves in both a leadership and clinical role. She has also been serving as a senior content expert and integrated behavioral health practice facilitator for CTC-RI for the past 4 years. Dr. Nelly Burdette received her doctorate degree in Health Psychology from Spalding University and completed her internship at Cherokee Health Systems, focusing on behavioral health services within a primary care safety net population. Her post-doctorate was completed at University of Massachusetts Medical School in Primary Care Psychology.
Course Participants: Behavioral health clinicians (PhD, PsyD, LICSW, LMFT, LMHC).
Course Start Date: March 1, 2020
Foundational Course Components:
- 4 online modules for self-study with reading and homework between modules
Module 1:
Overview of IBH Practice Facilitation and Core Competencies
Module 2:
The Primary Care and IBH Landscapes
Module 3:
The How-Tos of IBH Practice Facilitation
Module 4:
Evaluation in IBH Practice Facilitation
- Monthly calls with Dr. Burdette. Schedule to be arranged with Dr. Burdette
- Onsite at IBH pilot sites: Observation/supervision of trainee by Dr. Burdette. Schedule to be arranged with Dr. Burdette.
- A reference binder with readings for the course. CTC-RI will provide to every student.
- Continuing Education Credits approved by: NASW for 7 CEU credits
Estimated time commitment is ~24 hours.
Cost for Foundational Course: $750 for CTC members; $1000 for out of state
Advanced: Onsite IBH Shadowing (Optional) Highly recommended and unique add-on to the course includes a live shadowing component in which Dr. Burdette schedules your organization for an initial practice facilitation session with the course participant observing and then a follow-up practice facilitation session with Dr. Burdette shadowing the course participant. Shadowing rate is currently available to Rhode Island only, but please inquire if interested in out-of-state shadowing. Schedule to be arranged with Dr. Burdette.
Additional Cost for Onsite IBH Shadowing: $750
Interested course participants should submit their application and CV or resume to CTCIBH@ctc-ri.org by Feb 1, 2020. You will be notified of your acceptance and provided further instructions within 7 days of receipt.
Another Training program will be offered in the Fall of 2020.
Meeting Frequency
2nd Thursday Monthly
7:30-9:00AM
Topic focus on PCMH-Kids (Jan, Apr, Jul, Oct)
Topic focus on Adult IBH Pilot (Feb)
Committee Meeting (Mar, Jun, Sept, Dec)
The Integrated Behavioral Health (IBH) Committee is charged with supporting the development of, and ongoing learning around, sustainable approaches to integrating behavioral health in a wide variety of primary care practices. The IBH committee acts as content experts for informing the implementation of CTC IBH pilot projects and work in partnership with the health plans, systems of care, Office of Health Insurance Commission and other partners in testing and evaluating new models/programs of care. The committee acts as an advisory group to: a) inform Patient Centered Medical Home (PCMH) adult and pediatric practices and community health teams as they develop programs to meet the behavioral health needs of patient and families in primary care b) strengthen workforce development by coordinating efforts with academic programs c) inform public policy. The IBH Committee Charter can be found here (link to charter).
Resources
CODAC Behavioral Health Telehealth Operations Procedure
Overview of Commercial Payer Coverage for Telemedicine from OHIC
Blue Cross Blue Shield RI Telemedicine policy
UnitedHealthcare Telemedicine Resources
Optum Telemental Health Compliance Attestation
Neighborhood Health Plan Telemedicine policy
Tufts Commercial Telemedicine policy
Funding Sources:




PCMH Kids is a state-wide collaborative covering 110,000 children from 37 practice sites representing ½ the children in RI and 80% of the Medicaid population. This PCMH Kids IBH initiative consists of 8 pediatric practice sites serving approximately 40,000 children and represents both independent practice sites and practices that are part of systems of care. Priority was given to practices that serve vulnerable populations. This initiative recognizes and capitalizes on the fact that primary care is the logical center piece for providing effective mental health promotion and prevention because the pediatrician is the most likely medical professional that children and adolescents come in contact with during their early and adolescent years.
Through this pediatric IBH initiative, CTC-RI and PCMH Kids is building on its success in implementing integrated behavioral health in adult primary care practices as well as leveraging the behavioral health work done in pediatrics through our PCMH-Kids program over the past 3 years. The 8 pediatric practices enrolled in this program are:
Cohort 1 |
Anchor Pediatrics |
| Comprehensive Community Action Program (CCAP) | |
| Hasbro Pediatric Primary Care | |
| Tri-County Community Action Agency | |
Cohort 2 |
Coastal Medical – Bald Hill |
| Coastal Medical - Waterman | |
| Hasbro Medicine Pediatric Primary Care | |
| Northern RI Pediatrics |
Resources
Sample Practice Participation Agreement Cover Letter
Integrated Behavioral Health Agreement
Updated Measurement Specifications
Sample Job Description for PEDI IBHC
Sample Job Description and Interview Questions (from Starfish)
Sample Pediatric IBH Schedules
Center for Women’s Behavioral Health Referral Form
PEDIPRN letter & Enrollment Form
What Have We Learned Thus Far?
Providing Confidential Care to Adolescents in Healthcare Settings
Integrated BH Coding Guidelines
AAP Coding for Pediatric Preventive Care, 2019 - selected pages
Pediatric Symptom Checklist with Instructions
Edinburgh Postnatal Depression Scale
CRAFFT Screening Interview (updated version)
Brief Behavioral Therapy for Pediatric Anxiety and Depression in Primary Care
KIDS COUNT Children Mental Health Fact Sheet 2019
Funding Source:

CTC Sustainable IBH Objectives:
- To assist PCMHs within the CTC-RI network in recruiting and hiring an IBH provider for the primary care practice
- To increase the identification of patients across the lifespan with behavioral health and substance use disorders (SUD) through universal screening for depression, anxiety and SUD;
- To increase ready access to brief behavioral health intervention for patients with moderate depression, anxiety, SUD and co-occurring chronic conditions;
- To provide care coordination and intervention for patients with high emergency department (ED) utilization;
CTC is providing IBH practice facilitation to 9 primary care practices over a one year time period to assist them with implementing an IBH program geared towards providing holistic patient centered primary care services. The 9 primary care practices enrolled in the program are:
- Blackstone Valley Community Health Care
- Brown Medicine Primary Care – Warwick
- Charter Care Medical Associates – Lincoln
- Coastal Medical Providence Edgewood
- Providence Community Health Center – Central
- Providence Community Health Center – Crossroads
- Providence Community Health Center - Randall Square
- Tri-County Community Action Agency – North Providence
- Women’s Medicine Collaborative Primary Care
Resources
What Have We Learned Thus Far?
Addressing SDOC in PCP IBH Reimbursement Overview
Cheat sheet on Medicare Payments for IBH Services
Our Mission
The mission of the Care Transformation Collaborative is to lead the transformation of primary care in Rhode Island in the context of an integrated health care system; and to improve the quality of care, the patient experience of care, the affordability of care, and the health of the populations we serve.
